Health Net Mobile
Quick Reference Guide
- Registration
-
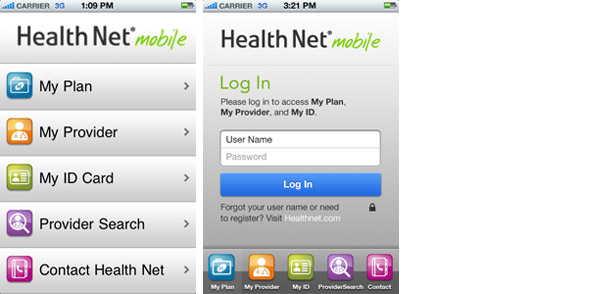
Health Net Mobile allows members to view plan details, provider information and a mobile ID card; utilize ProviderSearch; and find Health Net contact information.
Members must register a user name and password at www.healthnet.com to access:
- My Plan
- My Provider
- My ID Card
- The member search found in ProviderSearch
- ProviderSearch
-
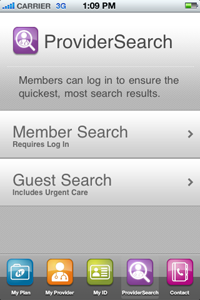 Health Net Mobile allows members to search for providers using ProviderSearch. ProviderSearch provides a guest search and a member search. The member search requires the member to log in and provides the most accurate search results.
Health Net Mobile allows members to search for providers using ProviderSearch. ProviderSearch provides a guest search and a member search. The member search requires the member to log in and provides the most accurate search results.
- Urgent Care Search
-
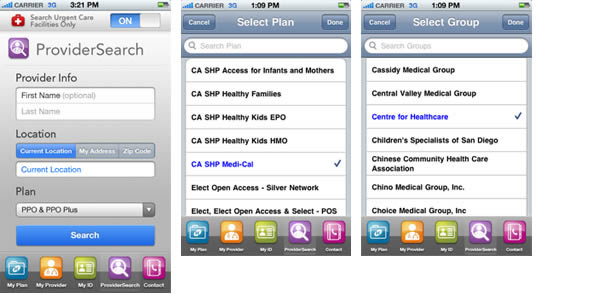
Users can search for urgent care facilities by sliding the indicator to "On".
When the "Search Urgent Care Facilities Only" indicator is "On", the provider name search is disabled.
Users can search by Current Location, My Address, or ZIP Code.
Current location will use the phone's native GPS tool to perform the search. My Address or ZIP Code will be pre-populated if the member is logged in.
Pre-login members will need to select a plan and a medical group if the plan is CA HMO.
- Search Results
-
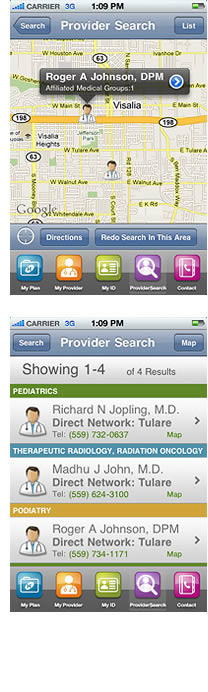 Search results can be displayed either in Map or List view. The default view is Map.
Search results can be displayed either in Map or List view. The default view is Map.Hovering over a search result will display basic provider information, such as the provider's name and the medical group the provider is affiliated with. Medical group information will only display for HMO members.
From the map view, the user can:
- Display the provider details screen by clicking the arrow.
- Find the user's current location on the map.
- Get directions to the provider's location by clicking the "Directions" button.
Note: Directions will be given based on the search option (current location, address, or ZIP code). The user can select to change the directions based on current location, home address or other location.
If the user clicks the List icon (top right corner), the search results are returned in a list.
The List view displays the number of results found and indicates the number of results currently being shown. If more than 20 results are returned, a “Load More Results” button will display.
Additional List view features include:
- Providers are grouped by specialty.
- If a provider has multiple specialties, the provider is listed under each specialty.
- Specialty groupings are separated by color.
- Phone number is a clickable link that launches the phone application.
- Map is a clickable link that launches the map and allows the user to get directions. Directions are given based on the search option (current location, address, or ZIP code). The user can select to change the directions based on the current location, home address or other location.
- Shows detailed information about the provider.
- My Plan
-
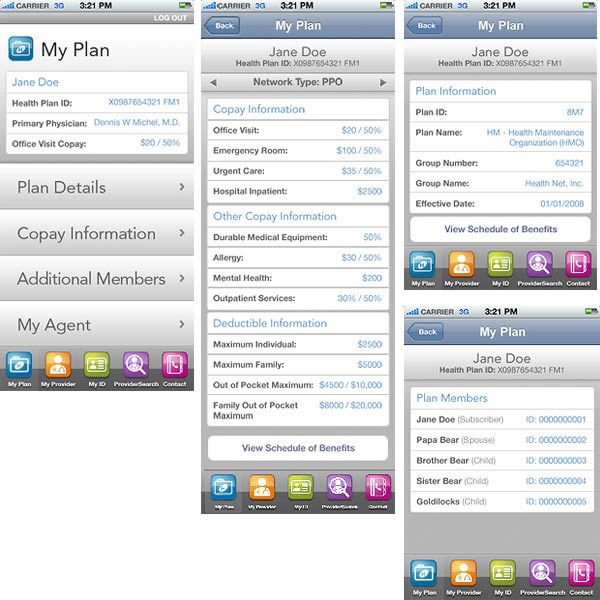
Members can view their specific plan information, and the Plan Details section provides members with information such as eligibility, plan name and effective date.
- My Provider
-
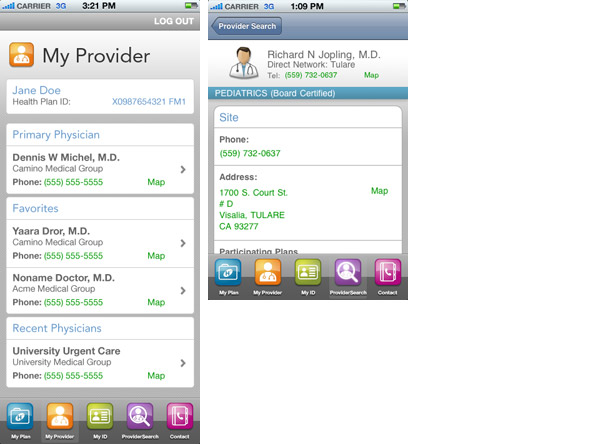
My Provider will allow a user to see specific provider information for any member on the plan.
- Primary physician – for HMO members only.
- Favorites – A Health Net Mobile feature. Providers can be added by clicking the “Favorites” link in ProviderSearch.
- Mobile ID Card
-
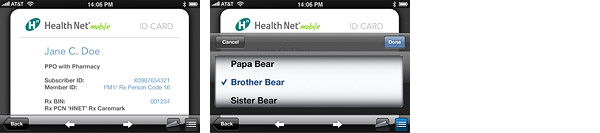
My ID Card provides the user with a mobile ID card.
Clicking the "Flip" icon will display the back of the card (front of the card if the member is on the back). If multiple members are on the policy, the signed-in user’s card will display first, and the user will have the ability to scroll all cards or view a list of members to select a different card.
- Contact Us
-
Health Net Mobile will provide the user with contact information and help topics.
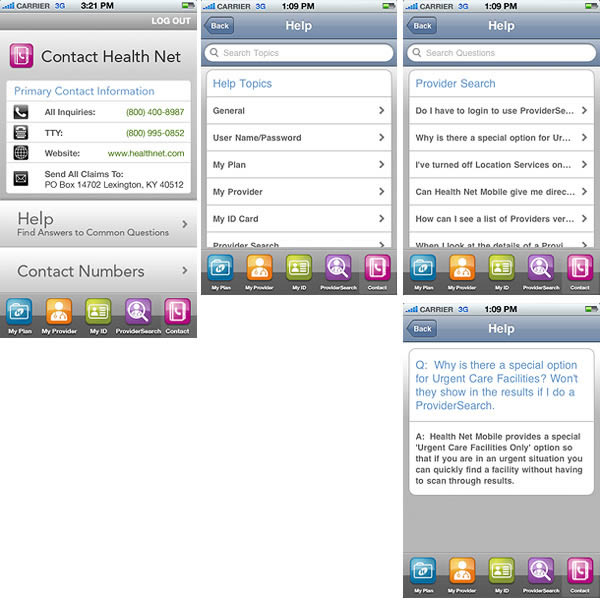
Contact Health Net provides users with phone numbers and a mailing address for claims. Logged-in members will see contact information specific to their plan. Users who access Contact Us pre-login will see region-specific information.
The Contact Health Net section also provides a help section where users can find information related to frequently asked questions (FAQs).
The help section is searchable, and questions are grouped by topic. To get more information about an item, select the topic and then select a question:
Health Net Mobile
Helpful Links
Download from the App Store
Download from Google Play
Access Mobile Web Version
Sneak Peek Video!
Quick Reference Guide
Mobile Help FAQs


















